ONLY SIX NATURAL HEALTH PRODUCTS PASS FIRST ‘COMPLEMENTARY MEDICINES’ PRE-REGISTRATION TEST
ONLY SIX HEALTH PRODUCTS PASS FIRST ‘COMPLEMENTARY MEDICINES PRE-REGISTRATION TEST
Anthony Rees
(Secretary-General TNHA)
‘Medicines Control Council inspectors are gearing up to seize scores of illegal products claiming to treat diabetes, heart disease, cancer and viral illnesses in a blitz aimed at enforcing tough regulations for complementary medicines’ – Business Day
The Medicines Control Council (MCC) gazetted a notice three weeks ago on the 15th of April in terms of section 14(3) of the Medicines and Related Substances Act (Act No. 101 of 1965).
This notice served to inform stakeholders, including the public, which current products are to be further considered for evaluation and possible registration with the Council as ‘Category D’ Complementary Medicines.
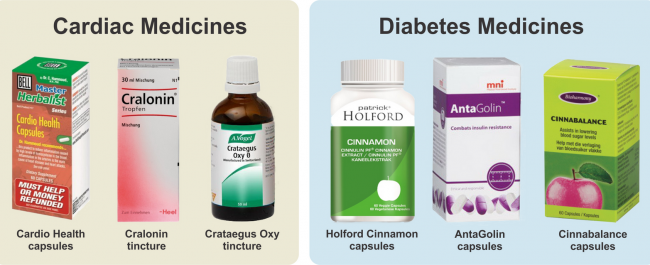
The only six products which the MCC are prepared to evaluate in terms of the first pharmacological classifications cited in the 2013-2019 Road Map.
In terms of the Road Map circular which was issued on the same day the complementary medicines regulations were gazetted on the 15th of November 2013, certain complementary medicines which were sold on the market on or before the regulations were published had to have applications for registration lodged on or before the 15th of May 2014.
The pharmacological classifications included:
- Antiviral agents
- Oral hypoglycaemics (remedies for diabetes)
- Cardiac medicines (remedies for heart conditions)
- Cytostatic agents (remedies for cancer)
It has been established that the Council received only 24 product applications for the above pharmacological classifications, and only 6 passed through the first cursory screening test for eligibility to be further tested for their safety, quality and efficacy.
No list has been made available of the other 22 products that were rejected or referred for registration as ‘Category A’ pharmaceutical drugs, or as ‘food supplements’.
This notice comes almost two years after the application for registration deadline set for these products. It is extremely concerning that we are rapidly reaching the half-way mark between 2013 and 2019 for all complementary medicines to be registered, and only six products have passed the first level of screening.
The MCC has a well-publicised historical backlog of registration applications in limbo due to severe capacity constraints. In a 2008 Ministerial Report on the restructuring of the Medicines Control Council, it was revealed that there are some 9 500 ‘Category A’ pharmaceutical drugs, of which many are risk substances, which have not been evaluated for their safety or efficacy, and yet they are allowed to be sold on the open market under a deal made with the pharmaceutical industry decades ago. Currently, the MCC takes as long as 2 to 5 years to get novel and generic pharmaceutical drugs on the pharmacy shelves.
Surely high risk novel drugs should be prioritised in assessment by the MCC, and not low risk natural health products which have not resulted in any recorded deaths in South Africa since the Medicines Act was promulgated over half a century ago? The disproportionate use of scarce resources to evaluate natural health products, and not significantly higher risk pharmaceutical products, is irrational and a gross dereliction of duty.
According to various statements by senior Medicines Control Council staff over the last few years, the MCC allegedly recorded approximately 18 000 natural health products in an audit they conducted between 2001 and 2011 [pg. 14 in link above]. Considering the snail’s pace of complementary medicine regulation thus far, it is highly unlikely they will be able to screen and approve all these products by 2019.
Having received a mere 28 applications out of potentially hundreds of products being sold with health claims associated with the pharmacological classifications above, it is clear the industry is unable to comply with the inappropriate and cost-prohibitive complementary medicines regulations imposed on the sector. Inadequate consultation, lack of transparency and vague and ambiguous regulations contribute to this paralysis. It is no wonder the industry, amanufacturers and distributors are boycotting the regulations en masse.
If any of the six products above pass the pharmaceutical assessment criteria set for complementary medicines, they will be awarded with a licence and registration number, thereby making them the only legal products for treating the above conditions.
All other products making health claims related to these pharmacological classifications, directly or through associated marketing materials, are now deemed illegal, and companies selling such products may face criminal prosecution. Only the six products mentioned may continue being sold, pending the finalisation of their assessments for registration.
We note that of the four pharmacological classifications listed, only two classifications have product applications listed in the notice, namely cardiac medicines and oral hypoglycaemics.
There were no successful applicants for natural antiviral or cytostatic (cancer) agents. What this means is that NO natural health products may be sold in the future which make claims (directly or indirectly) for treating viral infections or cancer.
For heart disease and diabetes sufferers, only three natural health products for each indication will possibly be allowed to be sold in future.
As this is only the first step towards the intended registration of these six products, the manufacturers and importers will have to tick all the boxes in further motivating their applications. This will include satisfying the vigorous requirements for testing new drugs for their quality (by being registered pharmaceutical manufacturers with pharmaceutical GMP certification), safety (through product screening), and efficacy to establish whether the health claims made are clinically substantiated (through product-specific research).
To jump these hurdles, companies will have to invest heavily in terms of capital expenditure (>R10 million) for production facilities, gather or conduct costly clinical research (costing tens of millions of Rand), hire costly regulatory consultants and hire full-time pharmacists as ‘responsible persons’.
Although this news is disheartening, the TNHA maintains that the entire regulatory process has been unconstitutional on the basis of discrimination (by not including African Traditional Herbal Medicine); it remains ultra vires (without an enabling clause in the principle Act for these products), irrational and procedurally unlawful.
The Registrar of Medicines, Dr Joey Gouws is on record in a recent Business Day article, stating that the Department of Health will soon begin enforcing the 2013 regulations and prosecute errant wholesalers who continue to sell unregistered natural health products making claims for the four pharmacological classifications above. She knows full-well that wholesalers have the least to lose by ceasing the distribution of these products, and will not risk losing their wholesale licences over a few complementary medicines. Manufacturers and importers, on the other hand, have much to lose by being prosecuted for selling illegal medicines and would most certainly defend their rights vigorously with the backing of their trade associations.
The trap most companies have fallen into is making disease reduction claims on their products and in associated marketing campaigns. This ensnares them into the broader definition of a medicine (drug) in terms of Section 1 of the Medicines and Related substances Act.
“medicine” means any substance or mixture of substances used or purporting to be suitable for use or manufactured or sold for use in –
- a) the diagnosis, treatment, mitigation, modification or prevention of disease, abnormal physical or mental state or the symptoms thereof in man; or
- b) restoring, correcting or modifying any somatic or psychic or organic function in man
and includes any veterinary medicine
This is exactly why the MCC are calling up natural health products in terms of previous pharmacological classifications previously established for pharmaceutical drugs.
The definition of a complementary medicine contained in the Nov 2013 regulations is similar, in that only when a health claim is associated with a product, does it become a medicine.
‘”complementary medicine” means any substance or mixture of substances that-
(a) originates from plants, minerals or animals;
(b) is used or intended to be used for, or manufactured or sold for use in assisting the innate healing power of a human being or animal to mitigate, modify, alleviate or prevent illness or the symptoms thereof or abnormal physical or mental state; and
(c) is used in accordance with the practice of the professions regulated under the Allied Health Professions Act, 1982 (Act No. 63 of 1982).
* Note the word ‘and’ at the end of (b), leading to (c). This definition makes it an explicit requirement for both (b) and (c) to be fulfilled to define a natural health product a ‘complementary medicine’. If no health claim is made for a product, it is not a medicine or complementary medicine.
A natural health substance product only becomes a medicine when (a) one or more of its ingredients have previously been declared a scheduled substance, or (b) it makes health claims.
If you are manufacturer or distributor of natural health products, and remove all health claims from your products and associated marketing materials, it does not fit into the definition of a medicine. You may simply state the name of the product and the list of ingredients it contains, in a similar way to which food are sold. Make sure your name does not infer a health claim either.
There are some in regulatory circles who argue that nothing escapes the broad definition of a medicine if the substance or product is ‘purported’ to have health promoting or healing function, whether scheduled or sporting health claims or not.
They claim the word ‘purporting to be suitable’ in the definition of a medicine renders most natural health substances registerable by being referenced in bibliographical records when they have been regulated as medicines elsewhere in the world.
The Oxford Dictionary defines the word purport as ‘appear to be or do something’. A product can only appear to do something if it claims to do something. To demonstrate the irrationality of this opinion, let’s look at some examples.
Water is used to prevent and treat dehydration, yet is not a registered medicine when drunk from a tap or as part of a beverage or in foods. Oxygen is used medically to assist patients with breathing complications, yet it is not a registerable medicine for breathing. Other examples include common herbs like garlic, parsley, turmeric, cinnamon etc. They are are all purported in the medical literature to have medicinal effects, yet they continue to be sold in any amounts without restriction in retail stores or even on the side of the street.
In law that any statutory health council, including the Medicines Control Council, is a creature of the particular statute which constitutes it, and that its powers are limited by the enabling legislative instrument (the Act). What the MCC is attempting to do is enforce the law by assumption and presumption based on their opinions. Their conduct and jurisdiction are ruled by certain explicit facts, namely the letter of the law in the Medicines and Related Substances Act. The word ‘purported’ in the definition of a medicine is both irrational and vague and has led to arbitrary decision-making.
